Nitin K Sethi, MD, MBBS, FAAN
You can reach me at: md.nitin@gmail.com
In this blog post, I shall discuss various treatment options for obstructive sleep apnea (OSA). Good news is that nowadays there are a number of very effective treatment options available for OSA. Let us discuss these one by one:
Positional Sleepers: This is the simplest treatment available for snoring and at times OSA. As the name suggests, a positional sleeper helps a person sleep on his/her side as against the back. Since snoring and OSA is frequently worse on the back, sleeping on the side is helpful (the tongue falls on the side and does not obstruct the flow of air). There are many different positional sleepers available on the market. Many of my patients design their own positional sleeper by using pillows or tennis balls sewn into their T shirt/PJs.

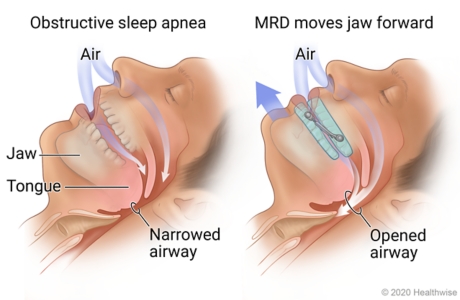
Mandibular Advancement Device (MAD): MAD is like a mouth guard. The patient puts the MAD into his/her mouth at night before sleeping. As the name suggests the device “helps to advance the mandible/lower jaw”. The tongue is attached to the lower jaw. So the device by pulling the jaw and tongue forward helps to make more room in the back of the throat for air to flow in and out more easily. There are MADs which are available over the counter. These devices while cheaper as compared to custom made device (made by a dentist) have one problem. They usually are not well fitting. As a result they are not comfortable and are not effective. The best MAD is one which is made by a dentist. The dentist measures the patient’s teeth and makes a device which fits well, is comfortable and effective. Most dentists make MADs so please talk to your dentist about this. There are dentists who are certified by the American Academy of Dental Sleep Medicine. In my opinion these dentists are the best in MADs and I frequently refer my patients to one.
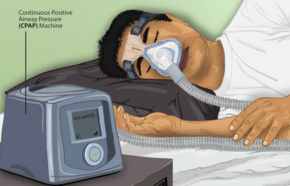
Nasal Continuous Positive Airway Pressure (CPAP): Nasal CPAP is the most effective treatment for OSA around the world. CPAP has no side effects-it is a simple machine which helps to “force” the air into the narrowed airway. The patient sleeps with a mask over the nose (nasal mask) or over the nose and mouth (full face mask). The mask is attached to the CPAP machine with the help of a long hose. In the night when the patient is about to sleep, he/she puts the mask on and turns on the machine. The machine sucks in room air, filters it (the machine can be fitted with HEPA filters), humidifies it (the machine has a small humidifier and the patient can change the setting to his/her comfort level) and then blows the air with force in to the patient’s nose. The machine does this throughout the night. In the morning when the patient gets up, the machine is turned off. Indeed a simple and effective solution to OSA. While nasal CPAP has no side-effects, there is one problem. That problem is that majority of patients initially find the CPAP uncomfortable to use. In my experience this is very common. I have patients who come back and tell me they hate the machine, they cannot sleep with the machine and that they will not use it. There are others who come back and say they love the machine and it has changed their lives. So, I tell my patients not to get dejected and upset when initially they are struggling with CPAP use. Finding the most comfortable mask, adjusting the CPAP pressure and humidifier settings wells and most patients over time begin to get used to sleeping with the machine and start to like it. The correct CPAP pressure (the pressure needed to make the OSA go away) is calculated in the Sleep Lab (patient sleeps in the Sleep Lab and while asleep the correct CPAP pressure is determined by the Sleep Medicine technician). There are numerous CPAP machines (different models made by different vendors) and many different types of masks. The trick in my opinion is to find the right mask for the patient and the correct CPAP settings. Once that is done, most patients like CPAP. I usually instruct my patients to try to use the CPAP as much as possible (goal is to get the patient to use the CPAP every night and throughout the night as many patients go to sleep with the CPAP on but then take it off during the night).
You must be logged in to post a comment.